Cancer Screening
Unlike diagnostic efforts prompted by symptoms and medical signs, cancer screening involves efforts to detect cancer after it has formed, but before any noticeable symptoms appear. This may involve physical examination, blood or urine tests or medical imaging.
Cancer screening is not available for many types of cancers. Even when tests are available, they may not be recommended for everyone. Universal screening or mass screening involves screening everyone. Selective screening identifies people who are at higher risk, such as people with a family history. Several factors are considered to determine whether the benefits of screening outweigh the risks and the costs of screening. These factors include:
- Possible harms from the screening test: for example, X-ray images involve exposure to potentially harmful ionizing radiation
- The likelihood of the test correctly identifying cancer
- The likelihood that cancer is present: Screening is not normally useful for rare cancers.
- Possible harms from follow-up procedures
- Whether suitable treatment is available
- Whether early detection improves treatment outcomes
- Whether cancer will ever need treatment
- Whether the test is acceptable to the people: If a screening test is too burdensome(for example, extremely painful), then people will refuse to participate.
- Cost
Recommendations
U.S. Preventive Services Task Force
The U.S. Preventive Services Task Force (USPSTF) issues recommendations for various cancers:
- Strongly recommends cervical cancer screening in women who are sexually active and have a cervix at least until the age of 65.
- Recommend that Americans be screened for colorectal cancer via fecal occult blood testing, sigmoidoscopy, or colonoscopy starting at age 50 until age 75.
- Evidence is insufficient to recommend for or against screening for skin cancer, oral cancer, lung cancer, or prostate cancer in men under 75.
- Routine screening is not recommended for bladder cancer, testicular cancer, ovarian cancer, pancreatic cancer, or prostate cancer.
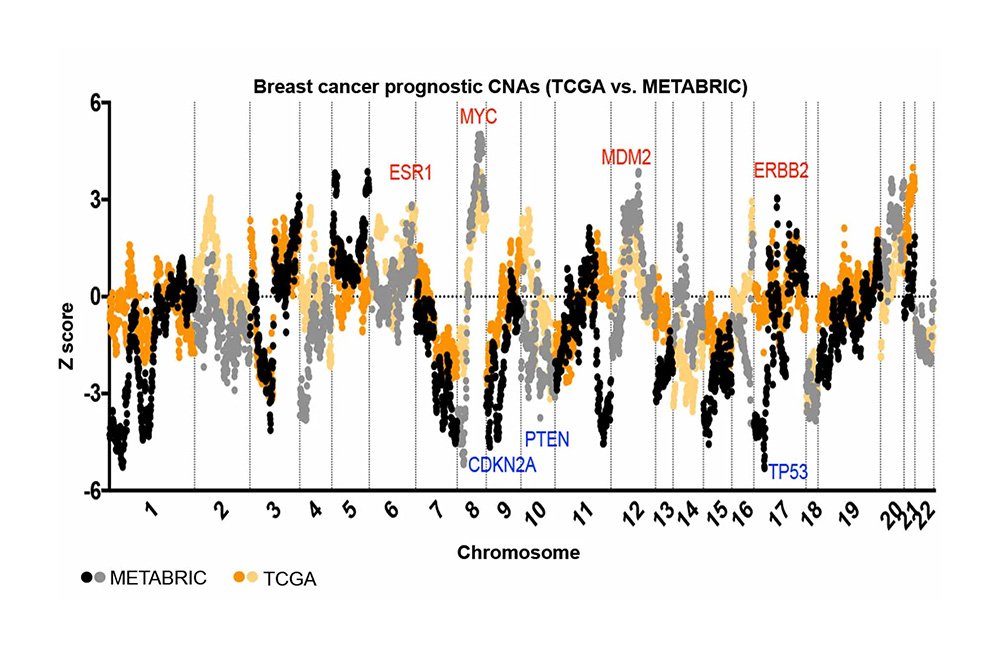
- Recommends mammography for breast cancer screening every two years from ages 50–74, but does not recommend either breast self-examination or clinical breast examination. A 2013 Cochrane review concluded that breast cancer screening by mammography had no effect in reducing mortality because of overdiagnosis and overtreatment.
Japan
Screens for gastric cancer using photofluorography due to the high incidence there.
Genetic Testing
| Gene | Cancer types |
|---|---|
| BRCA1, BRCA2 | Breast, ovarian, pancreatic |
| HNPCC, MLH1, MSH2, MSH6, PMS1, PMS2 | Colon, uterine, small bowel, stomach, urinary tract |
A coronal CT scan showing a malignant mesothelioma
Legend: → tumor ←, ✱ central pleural effusion, 1 & 3 lungs, 2 spine, 4 ribs, 5 aorta, 6 spleen, 7 & 8 kidneys, 9 liver